Pharmacy Benefit Managers: Specialty Medication Management and Contracting Trends
Highlights of the report:
Download a PDF of these Highlights
As pressure mounts to control specialty drug costs, PBMs are expanding their role across the value chain—placing greater emphasis on biosimilars, formulary strategy, and integrated capabilities. HIRC’s report, Pharmacy Benefit Managers: Specialty Medication Management and Contracting Trends, examines PBMs' involvement in specialty drug distribution, specialty medication management and formulary tactics, and trends in contracting with manufacturers. The report addresses the following:
- What are PBMs most focused on in 2026 to better manage specialty drug costs?
- What is the status of national recommended formularies and exclusion lists offered by PBMs?
- What drug categories are most targeted for additional preferred products and/or exclusions in future years?
- What is the status of PBM biosimilars adoption and current and future goals for private-label biosimilar offerings?
- What is the status of PBMs' copay adjustment program offerings? What is the status of PBMs' medical benefit management capabilities for clients?
- What is the nature of the contracting environment between PBMs and drug manufacturers?
- Which manufacturers stand out as best in PBM engagement to support their specialty portfolios?
Key Finding: Biosimilars are at the center of both PBMs' formulary strategy and contracting efforts in 2026. However, access is increasingly earned through partnership, not just price.
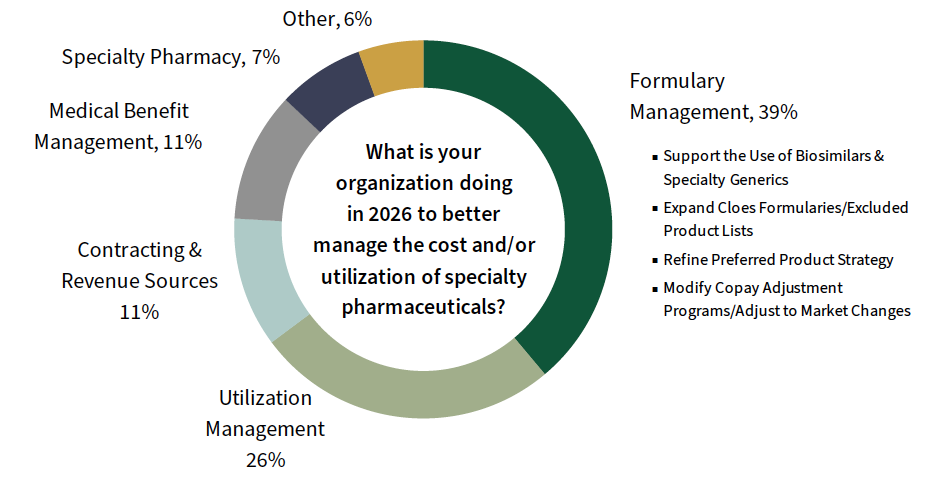
Biosimilars-forward Formularies Drive PBMs' Saving Efforts for Plan Sponsors. PBMs were asked to consider their top activities of focus to better manage the specialty drug trend for clients in 2026. Over one-third of activities center on formulary management for plan sponsors with a strong push towards leveraging biosimilars savings. PBMs also continue to leverage formulary exclusion lists. The full report examines PBMs' management activities in detail, as well as medical benefit management services and copay adjustment program offerings.
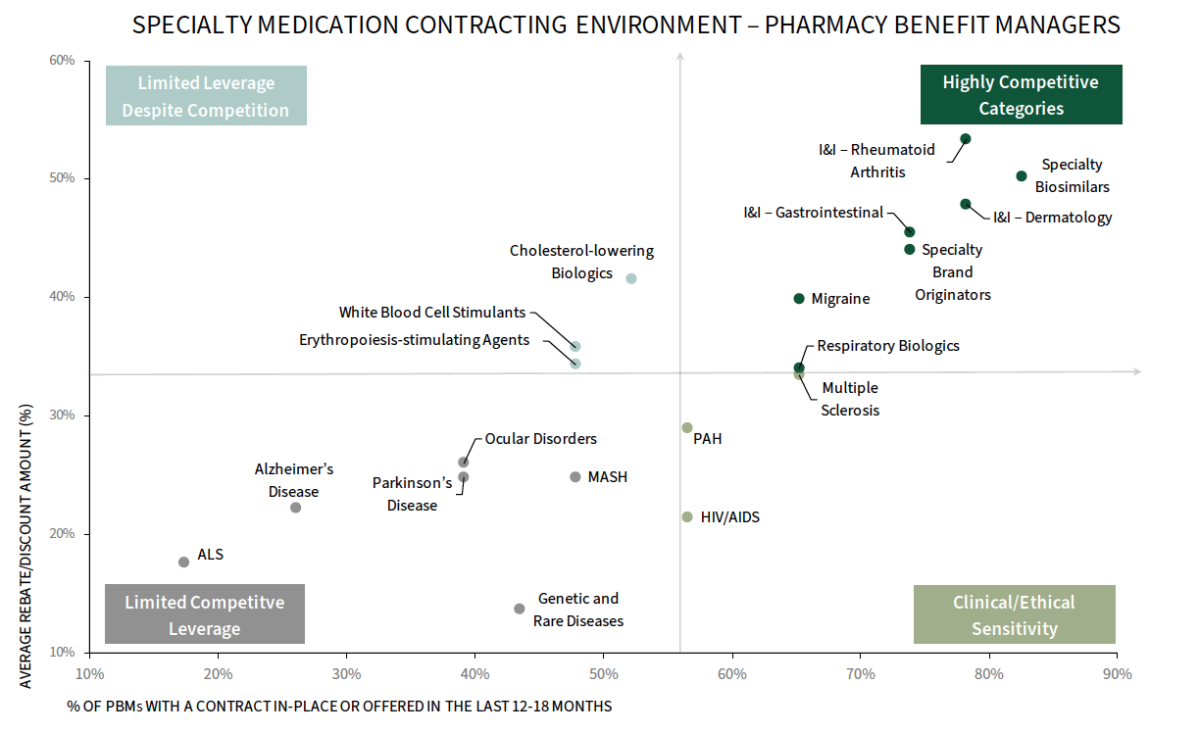
Rebates Remain Central to Contracting, but the Model is Evolving Amid Growing Policy Pressures. The below chart maps contract prevalence (share of PBMs with a contract in-place or offered) against average reported rebate levels across specialty therapeutic areas, showing where higher intensity contracting is observed–namely in competitive areas like I&I and biosimilars. The full report provides a deep dive into the contracting for the below therapeutic classes.
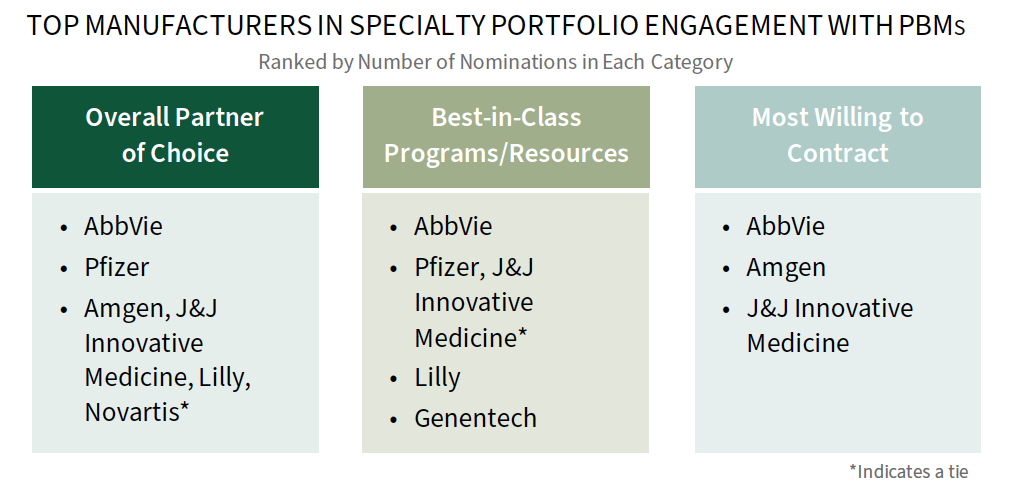
AbbVie Leads in Support of its Specialty Portfolio. PBM decision-makers were asked to nominate a manufacturer in three key areas as noted below. AbbVie is consistently among the leaders nominated in as best-in-class across categories, recognized for combining long-tenured, highly engaged account teams with flexible, PBM-aligned contracting. The full report also provides benchmark ratings of 35+ specialty medication manufacturers in presence and willingness to contract with PBMs.
Research Methodology and Report Availability. In February 2026, HIRC surveyed 25 pharmacy benefit manager decision-makers representing 13 unique very large, mid-size, and small/upcoming PBMs. Online surveys and follow-up telephone interviews were used to gather information. The Pharmacy Benefit Managers: Specialty Medication Management and Contracting Trends report is part of the Specialty Pharmaceuticals Service, and is now available to subscribers at www.hirc.com.
Download a PDF of these Highlights
Download Full Report (Subscribers only) >


